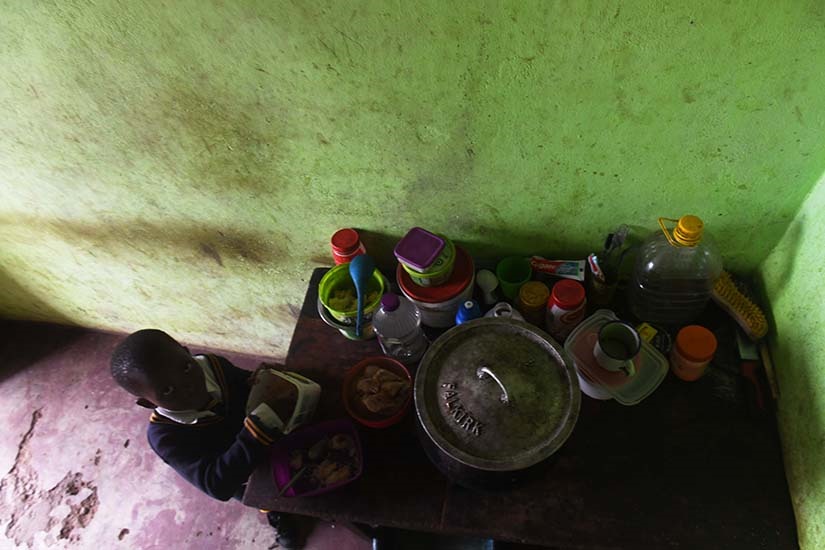Thabani is nine years old, and doesn’t have a pair of shoes.
His feet are calloused and dirty from walking to and from school and doing house work.
He lives alone with his 13-year-old brother in a rural village on the outskirts of Jozini, in the Umkhanyakude district in the far north of KwaZulu-Natal.
Their house is a small rondavel with an ageing roof that leaks when it rains, which is often.
But inside, there is little for the water to damage.
The biggest thing in the house is a 25kg bright orange bag of maize meal.
“It fills you!!!”, it states in bold lettering on the front of the bag.
An old red bicycle lays overturned on one side of the room, next to a table cluttered with Doom, toothbrushes, a few body cream containers and hangers.
Thabani’s older sister, Zanele, stays with extended family in another part of the village, but her school achievement award is placed next to these other items on the table.
The focal point of the house is the black cauldron in the centre of the room, on top of a thick pile of ashes and a few pieces of firewood.
Food is scarce for this child-headed family, living off only the basics of maize meal, sugar beans, potatoes and onions.
They have a refrigerator which is empty except for a few remaining beans still in last night’s pot.
The two boys are dependent on social grants that add up to less than R1 000 a month.
To supplement this, Thabani’s older brother pushes trolleys for customers at the shopping centre on the main road.
Thabani and his brother’s daily struggle against poverty and malnutrition is unfortunately quite common in the part of the world where they find themselves growing up.
Umkhanyakude has some of the worst child malnutrition numbers in all of the province’s districts, and KwaZulu-Natal fares worst among South Africa’s provinces.
Although things are particularly bad in places like Umkhanyakude, even in 2020 child hunger remains a global problem.
A landmark report of the World Health Organisation (WHO) and the Lancet medical journal published just last week found that “even in rich countries, many children go hungry or live in conditions of absolute poverty”.
Disturbing numbers
Children in about 753 000 households went hungry in KwaZulu-Natal in 2018, according to the 2019 Child Gauge (an annual publication tracking child health in South Africa).
This accounts for over a third of child hunger in South Africa and is two to four times higher than in any other province.
The high numbers are only partially explained by the fact that KwaZulu-Natal is South Africa’s second most populous province.
In the worst cases, hunger or malnutrition turns into so-called severe acute malnutrition (SAM). SAM is when a child’s weight for their height is below a certain threshold or when a child has a MUAC (mid-upper arm circumference) of less than 11.5cm.
Currently around 7.5% of children admitted to hospital with SAM in KwaZulu-Natal do not survive (a number referred to as the SAM fatality rate).
This is an improvement on the 7.8% in the province’s 2018/19 annual report, but still well behind the target of 6%.
According to the annual report 2 289 children were admitted to hospitals in the province for SAM in 2018/2019, of which 179 died.
It is not known how many children died of SAM outside of hospital or how many children died of other diseases like tuberculosis while also suffering from SAM.
The Umkhanyakude District has a SAM fatality rate of 11.4%, the highest in the province. In other words, one in 10 children admitted to hospital in the district with SAM do not survive.
Life in Jozini
Umkhanyakude’s district health office is in Jozini, the town where Thabani and his brother live. With unemployment at higher than 80%, and a quarter of the District’s child-headed households; Jozini is home to some of the country’s most vulnerable people.
Statistics SA’s 2019 estimate for the extreme food poverty line is R561 a month per person, but the child support grant falls R131 short, forcing children and families to live well-below this extreme line of poverty.
Light rain beats a steady pitter patter on zinc roofs of shops and fish and chips stalls in the centre of Jozini, where women carefully arrange large mangoes on colourful platters and bananas fresh from the trees.
The traffic moves constantly, both by car and by foot. Taxis own the road, along with the goats.
For most people the closest clinic is in the middle of town, while the newly opened Community Healthcare Centre is about 6km away across the Pongolapoort Dam bridge.
Bethesda Hospital is a 40-minute drive, and Mosvold Hospital is over an hour away in Ingwavuma.
Bethesda and Mosvold Hospitals are severely under-utilised according to the District’s 2018/19 health plan.
While Spotlight was refused permission to visit any clinics or hospitals in the area, our team spoke with community-based organisations who are leading the fight against child hunger and HIV/Aids in the area.
Siyaphambili Qondile
Siyaphambili Qondile has been providing care to communities in Jozini since 2000.
“We help people who are infected by HIV/Aids; taking them to hospital, referring them to [the social security agency] to apply for grants. It’s very difficult and we’ve been working [with] a bad situation because a lot of people were dying and leaving their children alone,” says Nokuthula Dladla, one of the organisation’s managers.
Siyaphambili has 15 community care workers and 19 child and youth care workers who work with families in Jozini and surrounding areas.
The organisation used to run a food parcel programme to support 30 families per month, but since 2015 hasn’t received funding for this programme.
Most of these food parcels went to child-headed households such as that of Thabani and his brother.
Siyaphambili social worker, Nonkululeko Buthelezi, says that often children between the ages of 10 and 13 spoke to her about facing hunger.
“The challenge we have now is for people to get food parcels. In the community we are living [in] people are suffering and others are taking treatment. They have no food, and closing the food parcel programme in our community is a challenge,” says Siyaphambili founder Musa Ndlovu.
“[Community members] come with their treatment and put it in front of you, what are you going to do? They even tell you, ‘I’m leaving this treatment because I don’t have food’,” says Ndlovu. “If I take this treatment, where am I going to get food because it makes me sick.”
Headless chickens
Care workers of Siyaphambili accompanied Spotlight on house visits in the community where poverty, hunger and malnutrition were severe issues.
In one household feathered chicken heads soak in a bowl of water next to a pot of maize meal as two children, Njabulo and Busisiwe, wait for their mother to return home.
Njabulo (7) and Busisiwe (13) are just two of five children in this one-room-house, with another one on the way.
The children sleep on woven mats on the floor with only a few blankets to share.
Their mother is out collecting firewood with two of the other children, one an infant, and the other a girl around Njabulo’s age.
The girl walks barefoot back up to the house in a sleeveless orange vest and shorts, her arms and legs worryingly thin.
There’s a slight breeze in the air. She shivers, rubbing her hands up and down her sides as she walks into the house.
The mother receives a disability grant of R1 700 a month for a mental health condition, but we are told she gives most of the money to her boyfriend.
The neighbours told Spotlight that because of this, the children do not get enough to eat nor personal hygiene items or clothing.
One of Siyaphambili’s care workers is concerned that Njabulo was malnourished and needed to go to the clinic for supplements. But the mother said that the children were always satisfied.
Ubombo Drop-In Centre
The Ubombo Drop-In Centre works with orphaned and vulnerable children as well as families who have been affected by HIV.
They run an Early Childhood Development (ECD) programme for 66 children, and provides meals to another 25 during after-school hours.
They also have 17 community care-givers which reach over 1 000 families.
Ubombo Project Manager Bheki Wilson Dube, tells Spotlight that community members struggle to take treatment for HIV and TB without food.
He says that in prior years protein porridge was distributed by the department of health, but this is no longer the case.
The department says that this project ended in 2017, but that it is currently under review.
“The issue of hunger is widespread throughout all the wards,” says Dube.
“That 66 [children in the ECD programme], most of them are identified as undernourished, not that severely because we are supplying them with food like corn flakes and Nespray [a powdered milk supplement], but come January you can see they are struggling,” he adds.
Zisize Educational Trust
Zisize Educational Trust in Ingwavuma, is another organisation working with children in the area as well as those affected by HIV/Aids.
Ingwavuma is about an hour from Jozini, and a mere six kilometres from the Swaziland border.
Be careful of the three “stop and go” roadblocks that either permanently say “stop” or “go” as you wind your way up through the Lebombo Mountains.
Zisize works with 14 schools in the greater Ingwavuma area, covering a near 60km radius.
The organisation provides educational and health outreach services to schools, and has 20 community care workers that visit families each month.
Zisize also runs a food parcel programme that provides for over 50 families each month, and counsels them on food security and nutrition.
As part of this programme, Zisize teaches community members how to grow their own food, which is a challenge in both Ingwavuma and Jozini as a result of water issues.
A shining light in the organisation is their orange Starfish Wellness Wagon, a child-friendly mobile clinic that visits primary schools four days a week for health screening.
The wagon is run by the organisation’s professional nurse, Nomsa Myeni and auxiliary nurse, Sizakele Dlamini.
“At schools it’s rare to get children with malnutrition,” says Myeni, “because even at schools they have feeding schemes.”
To test for malnutrition, Myeni and Dlamini take the child’s body mass index (BMI) and perform a MUAC test. If a child’s BMI and MUAC are below a certain level, the child is referred to the clinic for nutritional supplements. The child’s family is also evaluated by care workers for Zisize’s food parcel programme.
But Ingwavuma’s nutritional crisis only turned around in the last five years.
“It was really difficult, because the conditions were really bad,” says Dlamini.
“They were admitting, now and then, the malnourished children to hospital, it was so bad,” added Myeni.
Initiatives like the Wellness Wagon and Zisize’s food parcel programme have worked to improve nutrition in the area.
Unlike Jozini, there are six boreholes spread throughout villages in Ingwavuma and surrounds, making it easier for people to grow food and manage personal hygiene.
There are also community gardens and seed distribution programmes.
Government response
KwaZulu-Natal department of health spokesperson Agiza Hlongwane says that SAM is a complex problem stemming from both social and health issues.
“The health measures put in place to try to address this problem have focussed on three core actions: the promotion of breastfeeding, community based profiling for early detection of malnutrition and intersectoral support, and the implementation of WHO 10 steps for the inpatient management of severe acute malnutrition,” says Hlongwane.
According to the department two thirds of SAM fatalities occurred within the first year of life, and were attributed to poor infant feeding, poverty and food insecurity and comorbidity with HIV/Aids, TB or other conditions.
“Inadequate household food security results in undernutrition,” says Hlongwane.
“The role of the health sector here is to identify children with or at risk of undernutrition, treat the acute issues and link affected children and families to appropriate support systems especially the department of social development and the social security agency. We have a well-established referral system via hospital based social workers.”
To address child health concerns, the department established so-called Phila Mntwana centres to conduct early screening for health and nutritional issues. There are 54 of these centres in Umkhanyakude, but the District’s 2018/19 health plan states that their performance is poor.
The department notes the importance of the first 1 000 days, stating it “clearly highlights the urgency with which optimal nutrition practices should be implemented to achieve developmental goals and economic growth”.
Hlongwane also cites the National Integrated Nutrition Programme, which includes new ways of improving health through nutrition.
“This can be seen through the achievements in reducing the provincial severe acute malnutrition case fatality rate at hospital level, increasing Vitamin A coverage at community level and improvement in exclusive breastfeeding rates at all levels,” he says.
Triple burden
Spotlight previously published an article arguing that hunger, stunting and obesity were among the top issues to watch in children’s health for 2020, and experts are calling them the “triple burden”.
The new WHO/Lancet report states that “the so-called double burden of malnutrition means that overweight and obesity can coexist with undernourishment and micronutrient deficiencies within a single population”.
Put another way, the bright orange bag of maize meal in Thabani and his brother’s house might help fill their tummies, but does not meet their nutritional needs.
It seems clear that the levels of malnutrition seen in KwaZulu-Natal, and in the Umkhanyakude district in particular, will have long-lasting consequences both for the community and the individuals impacted directly – and it is the youngest who will be most severely affected.
“Poor foetal growth or stunting in the first two years of life leads to irreversible damage, including reduced adult height, lower attained schooling, and lower adult income,” states the new WHO/Lancet report.
“Children who are undernourished in the first 2 years of life and who put on weight rapidly later in childhood or in adolescence are at high risk of obesity and later chronic diseases.”
The Umkhanyakude District health office was approached for comment but did not respond by the time of publication.
*Children and adolescent names have been changed in this article for both the privacy and dignity of the families.
See the WHO’s guidelines on SAM here.
**Spotlight would like to thank each of the organisations for their time, as well as the Maputaland Community Radio Station in Jozini for their assistance.
 | ||||||||||||||||||||||||||
Get in touchCity Press | ||||||||||||||||||||||||||
| ||||||||||||||||||||||||||
| Rise above the clutter | Choose your news | City Press in your inbox | ||||||||||||||||||||||||||
| City Press is an agenda-setting South African news brand that publishes across platforms. Its flagship print edition is distributed on a Sunday. |




 Publications
Publications
 Partners
Partners